The Electrodiagnostic Test (AKA “EMG”); The What, Why and When

Summarize with AI
by Puneet Ralhan DO and Susan Sorosky MD
The art of medicine lies in the ability to listen to a patient’s history and perform a comprehensive physical examination in order to arrive at an accurate diagnosis. Modern medicine has progressed to include new technology that helps us gain more information to diagnose various conditions. One such tool is the Electrodiagnostic Test, commonly referred to as an “EMG,” which is comprised of two parts – Nerve Conduction Studies (NCS) and Electromyography (EMG). This test evaluates the function of nerves and muscles. Physicians trained in performing this test include Board-Certified Physical Medicine and Rehabilitation specialists including the physicians at Desert Spine and Sports Medicine as well as Neurologists.
THE WHAT:
The two parts of Electrodiagnostic Testing – NCS and EMG – are performed together at the same visit. The entire evaluation typically takes between 30 minutes to an hour depending on the complexity of the condition. While a test involving small electrical stimulations and an acupuncture sized needle may sound painful, it is important to note that the overwhelming majority of patients tolerate the test well.
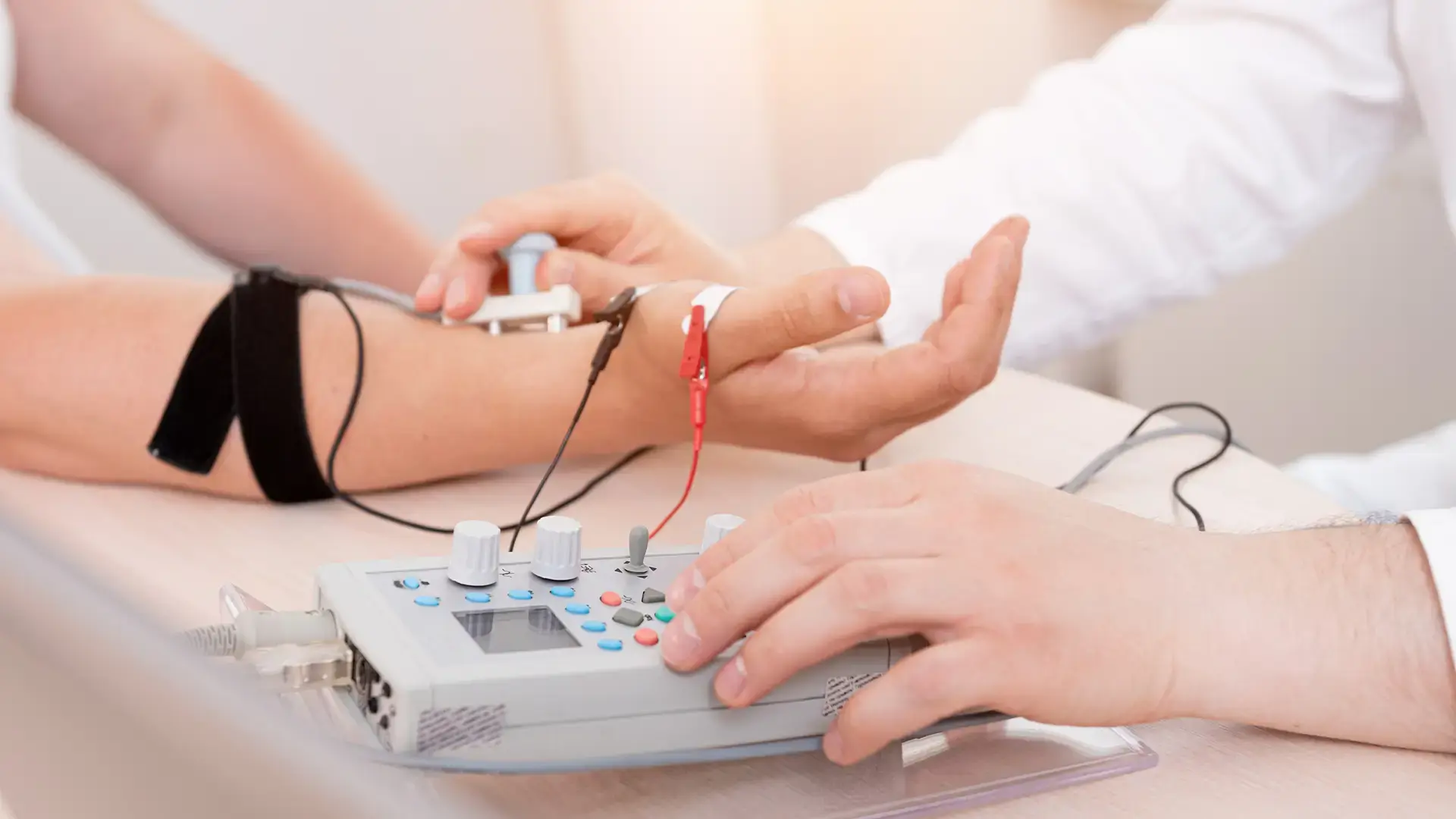
Nerve Conduction Studies (NCS): This portion of the exam is performed by using a stimulator device to deliver low intensity electrical impulses to the nerves which are then picked up by electrode stickers applied to the skin. These electrodes translate these signals into graphs and numerical values displayed on a computer which are analyzed by the specialist. The NCS is not painful, but patients often report feeling twinges (small brief electrical shocks) or muscle twitches.
Electromyography (EMG): During this part of the test, a needle electrode, a small thin needle about the size of an acupuncture needle, is inserted superficially into a muscle to record the electrical activity in that muscle. During this test, muscles are evaluated both at rest and with slight contractions. This specialized needle transmits sounds and unique waveforms to the computer which are analyzed by the physician. While the needle electrode may cause mild discomfort in some muscles, this ends quickly and does not typically persist after the needle is removed.
THE WHY:
Electrodiagnostic testing is helpful in the evaluation of diagnoses involving nerve or muscle damage including patients presenting with limb pain, numbness and tingling, and weakness. Pathology can happen in any part of the peripheral nervous system – from the spinal cord to the spinal nerve to the plexuses to the peripheral nerves – or in the muscle. An EMG can help pinpoint the location and severity of the damage, differentiate between acute and chronic injury, determine neurological recovery, and prognosticate outcome. Some of the most common conditions we evaluate in our clinic include:
- Lumbar radiculopathy
- Cervical radiculopathy
- Brachial/lumbar plexopathy
- Carpal tunnel syndrome
- Ulnar neuropathy/Cubital tunnel syndrome
- Peripheral nerve entrapment
- Peripheral Neuropathy
- Myopathy
THE WHEN:
When ordering an EMG to evaluate nerve damage, it is important to remember that timing is generally important. This is true because the degree of muscle denervation that occurs after nerve injury cannot be determined until Wallerian degeneration (the disruption of the myelin and axons along the entire length of the nerve below the site of the lesion) is complete. This process can take anywhere from 1-4 weeks to occur depending on the length of the nerve affected (longer nerves take more time). Therefore, in order to get complete data from an EMG, it is better to wait at least 2-3 weeks from the onset of nerve damage/injury before performing this test.
IN CONCLUSION;
Electrodiagnostic testing is a low-risk procedure, and complications are rare. It is important, however to inform the specialist performing the test if the patient has a pacemaker, defibrillator or any other electrical medical device, takes blood-thinning, or has a blood clotting disorder.
As board-certified specialists in Physical Medicine and Rehabilitation (PM&R), we are experts at diagnosing and treating problems affecting the nerves, muscles, soft tissues and bones. Here at Desert Spine and Sports Physicians, we take the time to accurately pinpoint the source of a problem through taking a detailed medical history and performing thorough musculoskeletal and neurological examinations. In addition, we have expertise in interpreting pertinent imaging studies (i.e. X-rays, MRIs, CT scans), and performing Electrodiagnostic Testing for diagnoses involving nerve and muscle. By combining information on structure (imaging) and function (EMG), we are able to identify a specific pain generator so we can then implement a specific treatment plan. If you have any further questions, feel free to contact us at Desert Spine and Sports Physicians for a full consultation to see if this test is right for your patient.
Additional Reading
Exploring Electrodiagnostic Testing: A Key to Diagnosing Nerve and Muscle Disorders
Tackling Sciatica and Radiculopathy: Non-Surgical Treatment Options
What Are Epidural Steroid Injections: A Patient’s Guide




.png)